

Monthly Archives: September 2016
Esther’s Birthday Dinner
AM Report 9/27/2016 – Graves Disease
Causes of High Output Heart Failure:
– Obesity (most common ~ 31%)
– Systemic AV shunts (22.5%)
– Hepatic disease (22.5%)
– Lung disease (i.e. COPD ~ 16%)
– Myeloproliferative disorders (multiple myeloma, myelofibrosis)
– Sepsis/Fever
– Hyperthyroidism
– Anemia
Hyperthyroidism
Presentation:
Increased thyroid hormone → increased metabolism → decreased SVR → increased cardiac output → increased contractility of heart muscle → increased myocardial oxygen demand/consumption
Physical Exam:
– tachycardia / atrial fibrillation
– hyperdynamic precordium
– systolic hypertension with widened pulse pressure
– brisk carotid/peripheral arterial pulsations
– loud first heart sound
– fine tremor
– warm moist skin
– exophatalmos (occurs in 20-25% of Graves patients)

– pretibial myxedema

Treatment:
– return patient to euthyroid state with antithyroid medication or RAI
– caution BB use – can reduce myocardial contractility in patients with impaired LVSF
Radioiondine Uptake Scan Interpretation:
Normal/Elevated Uptake:
[Autoimmune] – Graves disease, Hashimotos thyroiditis
[Autonomous Thyroid Tissue] – Toxic adenoma, toxic multinodular goiter
[TSH-mediated] – pituitary tumor
Low/Absent Uptake:
[Thyroiditis] – de Quervain’s thyroiditis, radiation thyroiditis, amiodarone thyroiditis
[Exogenous Thyroid Hormone] – excessive replacement, factitious hyperthyroidism
[Ectopic Hyperthyroidism] – Struma ovarii, metastatic follicular thyroid cancer
AM Report 9/26/2016 – Malaria
Malaria
Transmission: Anopheles mosquito (nighttime bites)
Cause: Protozoan parasite (5 types) – P. falciparum, P. vivax, P. ovale, P. malariae, and P. knowlesi
Clinical Presentation: fever, headache, chills, vomiting – can progress to severe illness/death
Incubation Period: variable 12-14 days (early) to months
Diagnosis: Thick/Thin smear (gold standard), RDTs, PCR, serology/IFA (NOT FOR ACUTE DIAGNOSIS)
Treatment: Depends on uncomplicated vs. severe, suspected species, and drug-resistance

* Remember that P. vivax and P. ovale can remain dormant for months/years in your liver (hyponozoites)
* Remember to test for G6PD before administering primaquine given the risk for hemolytic anemia
* Negative Duffy blood group is protective against P. vivax – since it requires the Duffy antigen for cell entry.
Dengue Fever
Transmission: Aedes mosquito (day and night bites)
Cause: viral infection (Dengue single-stranded RNA virus 4 serotypes)
Clinical Presentation: Maculopapular rash on face, thorax, and flexor surfaces, abdominal pain, nausea/vomiting, diarrhea, saddleback fever – fever abates for a day and returns
Incubation Period: 3-14 days; >2 weeks UNLIKELY to be dengue
Diagnosis: IgM capture ELISA – serologic assay, viral RNA, NS protein-1 antigen
Treatment: Supportive care; self-limited illness
Chikungunya
Transmission: Aedes mosquito (day and night bites)
Cause: Viral infection (Chikungunya virus – arbovirus)
Clinical Presentation: Fever, joint pain (common); headache, muscle ache, joint swelling, rash
Incubation Period: 3-7 days after infection
Diagnosis: IgM anti-chikungunya ELISA
Treatment: Supportive care; self-limited illness
Typhoid Fever
Transmission: Fecal/oral from infected humans
Cause: Bacteria: Salmonella Typhi
Clinical Presentation: High fever, weakness, abdominal pain, constipation (early) followed by diarrhea (later), salmon/rose-colored rash, HSM
Incubation Period: 8-14 days usually; can range from 3 days to 1 month
Diagnosis: Culture blood/stool/bone marrow for S. Typhi; serologic testing for S. Typhi antibodies
Treatment: Flouroquinolones (resistance growing), ceftriaxone, azithromycin
AM Report 9/22/2016 – Cauda Equina Syndrome
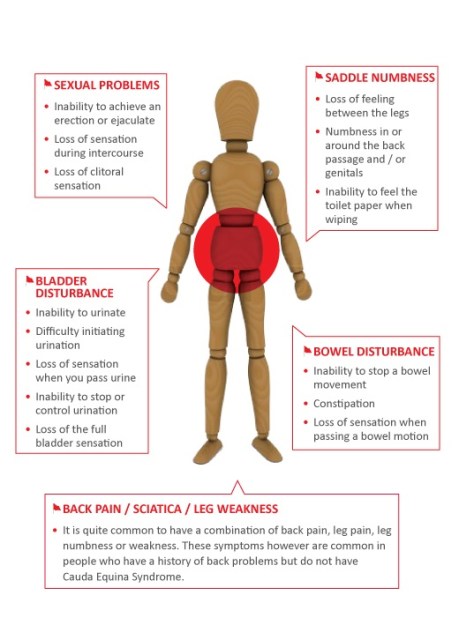
Cauda Equina Syndrome:
Cauda Equina: set of intradural nerves that provide sensory/motor innervation from L2-S5
Nerve Roots of Cauda Equina:
- Hip muscles
- Lower extremity muscles
- Urinary and anal sphincters
- Sexual organ muscles
Causes of Cauda Equina:
- Disc herniation (MOST COMMON)
- Lumbar stenosis (OA)
- Trauma
- Infection/abscess
- Metastatsis/neoplasma (Metastasis most common, ependymoma or schwannoma possible)
- Inflammatory disease (CIPD, Paget’s, ankylosing spondylitis)
Symptoms – based on level
Low back/radiating LE pain with at least one below
- Urinary incontinence/retention
- Fecal incontinence/retention
- Loss of anal sphincter tone
- Sexual dysfunction
- Saddle anesthesia/hypoesthesia
Treatment:
– urgent neurosurgical evaluation to reduce side/eliminate mass
– eradicate causative organisms
Most common organisms:
– staph (63%)
– strep (9%)
– gram negative anaerobes (16%)
Empiric antibiotic regimen: vancomycin and cephalosporin +/- nafcillin
Steroids indications:
– within 8 hours of traumatic spinal cord injury
– metastatic disease (followed by surgery/radiation)
9/20/2016 AM Report – Cannabinoid Hyperemesis Syndrome
Cyclic Vomiting Syndrome
Define:
- Stereotypical episodes of vomiting <1 week
- 3 episodes in past year, 2 in past 6 months, at least one week apart
- Absence of vomiting between episodes
3 Phases – Interepisodic, Prodromal, and Vomiting
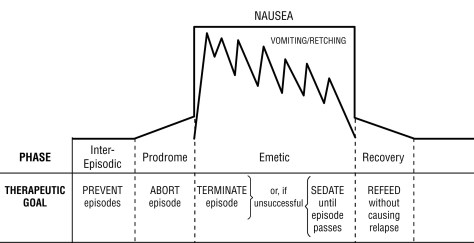
Epidemiology:
- More common in children
- More frequent bouts in children (12/year) vs. adults (4/year)
- Broad age of onset for adults
- Symptoms longer for adults prior to diagnosis
- Nausea between episodes is more common in adults
Differential diagnosis:
ACUTE:
- Acute gastroenteritis (rotovirus, enteric aderovirus, norovirus)
- Post-operative nausea/vomiting
- Vestibular neuritis
- Chemotherpy/Drugs
CHRONIC:
- Pregnancy
- Chronic nausea/vomiting syndrome
- Gastroparesis
- Gastric outlet obstruction
- CVS
- Rumination syndrome
Cannabinoid Hyperemesis Syndrome
Define:
- Stereotypical episodic vomiting similar to CVS (onset, duration, frequency)
- Presentation after prolonged/excessive cannabis use
- Relief of symptoms with sustained (1 week) cessation of cannabis*
* often associated with pathologic bathing behavior (prolonged hot baths/showers) – considered pathognomonic for CHS
9/7/2016 AM Report – IgA Nephropathy
Nephrotic Syndrome:
Define:
– Proteinuria (>3.5 g/24h or urine/creatinine > 3.5 mg/mg)
– Hypoalbuminemia
– Clinical evidence of edema
* Other clinical manifestations (hyperlipidemia, coagulation abnormalities) are related to losses of proteins other than albumin or caused by increased protein synthesis.
Nephrotic Range Proteinuria: > 3 g/24h without other findings
Nephritic Syndrome:
Characterized by: proteinuria, hematuria, pyuria, and often decreased kidney function and hypertension
– due to injury or inflammation within the glomerulus that allows the passage of protein, erythrocytes, and leukocytes into the renal tubule.
– resulting damage can lead to decreased GFR, kidney function, and abnormal blood pressure
IgA Nephropathy:
– most common primary glomerulonephritis
– an immune complex disease in which IgA antigen-antibody complexes are depositied primarily in the mesangium
– may be primarily involve the kidney or may be secondarily associated with other conditions
Epidemiology: occurs at any age, but usually found in men (20-30 yo) who are white or Asian
– develops to ESRD in approximately 20-30% of patients within 10-20 years of onset
Risk factors for progression: younger age at onset, hypertension, proteinuria > 1 g/24h, elevated creatinine, and low GFR
Clinical manifestations:
– typically asymptomatic at presentation with only microscopic hematuria and proteinuria on urine evaluation
– common presentation: recurrent gross hematuria occuring synchronously with an episode of respiratory or GI infection
Diagnosis: confirmed by kidney biopsy
Management: ACE inhibitors or ARBs, with goal urine protein excretion < 1 g/24h
Simplified Approach to GN:
Step 1: determine the broad cause of the acute or progressive renal failure
– Pre-renal, intrinsic renal, or post-renal
– FENa (if oliguric to differentiate pre-renal from ATN), UA (evaluated for sediment), and renal US (rule out obstruction)
– If INTRINSIC renal than the differential is either: Glomeruli, Tubules, Interstitum, Vessels
Step 2: If a glomerular cause – differentiate between GLOMERULONEPHRITIS pattern from a NEPHROTIC SYNDROME pattern
– UA, renal US, 24 hour urine protein (urine protein:creatinine ratio)
– Look for active sediment (UA with protein and RBCs, dysmorphic RBCs, and/or RBC casts)
Step 3: Use the serum complement levels to differentiate cause of GN
Low Complement GN:
Systemic: SLE, endocarditis, cyroglobulinemia
Isolated Renal: post-infectious GN, MPGN
Normal Complement GN:
Systemic: HSP, ANCA-associated, Goodpasture’s syndrome, hypersensitivity vasculitis
Isolated Renal: IgA nephropathy, anti-GBM disease, RPGN
09/12/16 AM Report: Mesenteric Ischemia
Remember to distinguish ACUTE mesenteric ischemia from CHRONIC mesenteric ischemia, can sometimes see Acute on Chronic ischemia.
Acute: SUDDEN onset abdominal pain due to intestinal hypoperfusion ~50 % mortality if not treated
Chronic: gradual chronic abdominal pain due to intestinal hypoperfusion (intestinal angina)
Etiology (Acute): Arterial embolism (eg: dislodged thrombus from LA/LV/cardiac valve, septic emboli from IE, hx of A.fib not on anticoagulation), or arterial thrombosis.
Etiology (Chronic):Most common cause of chronic mesenteric ischemia is atherosclerosis, commonly affecting SMA or celiac arteries
Risk factors: History of atrial fibrillation, atherosclerotic disease (CAD, MI, PAD, smoking, DMII), for chronic mesenteric ischemia, age>60, female 3x>male, smoking, 50 % of patients with CAD, CVA, PAD
Acute mesenteric ischemia S&S: pain out of proportion to exam, severe pain, guarding (no time to form collaterals!), nausea/vomiting
Chronic mesenteric ischemia S&S: recurrent episodes of acute abdominal pain after eating, can lead to weight loss: Triad includes postprandial pain,food phobia , and weight loss.
Diagnosis: CTA has high sensitivity/specificity, can also use Duplex ultrasound but more variability in sensitivity as operator dependent
For chronic mesenteric ischemia, must see high grade mesenteric vascular stenoses in at least 2 major vessels (usually one vessel alone will
Treatment of ACUTE mesenteric ischemia: broad spectrum abx, anticoagulation (heparin), open embolectomy, aorto-mesenteric bypass, laparotomy to remove necrosed bowel, and use of Vasodilators if non-occlusive.
Treatment of CHRONIC mesenteric ischemia: supportive care, if severe symptoms, can do revascularization with angioplasty +- stenting, aorto-mesenteric bypass
Comparing Mesenteric Ischemia and Ischemic Colitis

09/08/16 AM Report-Amyloidosis
Etiologies for Restrictive Cardiomyopathy
Idiopathic
Endomyocardial fibrosis, Loeffler eosinophilic endomyocardial fibrosis
Secondary restrictive cardiomyopathy
Infiltrative-Hemochromatosis, Amyloidosis (most common cause of RCM in the USA), Sarcoidosis
Other: Radiation induced, Anthracyclines (eg: Doxorubicin), Malignancy, Glycogen storage diseases, Systemic sclerosis
Etiologies for Constrictive Pericarditis
Idiopathic, viral pericarditis, Tb (most common worldwide), connective tissue disorders, uremia, neoplasms, drugs (eg:Procainamide/Hydralazine)
Restrictive Cardiomyopathy vs. Constrictive Pericarditis
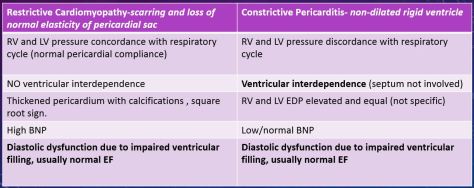
Amyloidosis-remember that it is a systemic disease!
- RENAL (# 1 MC): proteinuria (usually nephrotic range)
- CV (#2 MC): cardiomyopathy (restrictive), arrhythmias, angina, low voltage on EKG with pseudo-infarct pattern
- GI: Hepatosplenomegaly, gastroparesis
- NEURO: Peripheral/autonomic neuropathy, median nerve compression (carpal tunnel), orthostatic hypotension
- MSK: pseudo hypertrophy of muscles, macroglossia with lateral scalloping, amyloid arthropathy (thickening of synovial membrane)
- HEMATOLOGIC: Decreased Factor X activity (increased risk of bleeding)
- PULM: Tracheobronchial infiltration most common, pleural effusion, rare to have Pulm. HTN
- SKIN: easy bruising (ecchymosis), periorbital ecchymosis (“Racoon Eyes”) that is worse with Valsalva maneuvers, nail dystrophy, Alopecia,
Making the diagnosis
- Start with fad pad biopsy due to low risk of bleeding but if negative, may need to biopsy affected organs to make diagnosis. Stain with Congo Red stain and look for Apple-Green birefringence under polarized light to make diagnosis
- Most common cause of Amyloid in the USA is AL Amyloid-clonal expansion of plasma cells in the bone marrow that secrete a clonal Ig Lambda chain that deposits as amyloid fibrils into tissues, can occur with or without multiple myeloma, including with non-Hodgkins lymphoma and Waldensrom’s macroglobulinemia
- Check immunofixation and free light chain assay (SPEP/UPEP can be falsely negative)
09/06/16 AM Report: PCP Pneumonia in HIV patients
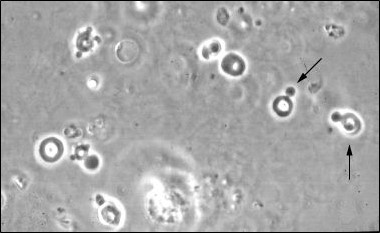
Pneumocystis jirovecii (previously Pneumocystis carinii)
Problem script
Epi: immunocompromised (eg: HIV with CD4<200 or not on Bactrim PPX, hematologic malignancy s/p BMT)
Timing: Sub-acute (weeks)-contrast with acute bacterial PNA which is more acute!
S&S: Fever (>80 %), progressive exertional dyspnea (95 %), non-productive cough, CXR usually with bilateral infiltrates but can also cause PTX, can also see GGO on CT scan
Labs to support diagnosis but does not make the diagnosis
Elevated LDH (sensitive but not specific)
ABG-check degree of hypoxia and AA gradient
Elevated 1,3 beta-d-glucan-part of cell wall (sensitive but not specific)
HIV with CD4 count <200 (risk factor)
Imaging
CXR-classically bilateral interstitial/alveolar infiltrates but can be variable. Suspect PCP if spontaneous PTX in patient with PNA and risk factors for PCP!
CT–excellent sensitivity, can see bilateral patchy/nodular ground glass opacities (not necessary but can order CT if unclear diagnosis)
Making the diagnosis– must VISUALIZE cystic/trophic forms, PCP cannot be cultured
Step 1: Sputum Induction (order specifically for PCP!), specificity of ~100 % but variable sensitivity of 55-90 %
If negative and high suspicion for PCP, proceed to Step 2
Step 2: Bronchoalveolar Lavage, 90-100 % sensitivity, ~100 % specificity
Treatment
First line is Bactrim 15-20 mg/kg oral or IV TID/QID x 21d (remember Bactrim has good bioavailability!)-No need to hold treatment before making diagnosis if high suspicion!
Treat with adjunctive steroids if PaO2<70 or A-A gradient >35
Dosing: Prednisone 40 mg PO BID x 5d, 40 mg PO daily x 5d, 20 mg PO daily x 11d.
Remember that it can take several days to see response in treatment, can get worse before getting better!
Primary Prophylaxis in HIV patients







