Today we discussed a case of an unfortunate young man who presented with chest tightness and syncope who later was found to have a massive PE.
We first discussed that the PE risk stratification is, by no means standardized and that every single society guideline differs slightly. Furthermore, an algorithmic approach is never 100% sensitive and an overall gestalt is valuable.
A. Risk Stratification per ACP from their clinical guidelines, published in 2015 in Annals
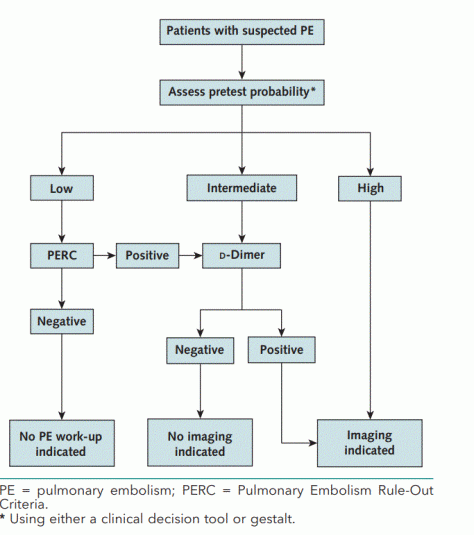
B. Once a PE is diagnosed, we emphasized the need to classify patients based on the following framework:
- Massive PE
- Hypotension is defined as a systolic blood pressure <90 mmHg or a drop in systolic blood pressure of ≥40 mmHg from baseline for a period >15 minutes or hypotension that requires vasopressors or inotropic support and is not explained by other causes
- Submassive PE
- Electrocardiographic Signs of Right Heart Strain
- Echocardiographic Signs of Right Heart Strain
- Biomarkers of Heart Strain
- Nonmassive PE
Remember, the anatomic location of the embolus does not relate to the above classification (i.e in a saddle embolus, a retrospective analysis found that only ~22% of such patients had hemodynamic instability)
B. Treatment of PEs
- Nonmassive PEs will be anticoagulated
- Regarding massive PEs, treatment patterns vary depending on the institution – but generally speaking –thrombolytics are first line. Depending on the patient and expertise, mechanical thrombectomy and catheter-directed lysis are also possibilities
- The controversial area is the submassive PE
- There is no standardized approach to submassive PEs, and even more complicated is that there is no consensus on what exactly is submassive. As Dr. Gohil said, there is submassive and there is submassive. Our goal as internists is to identify patients on teethering death. See this phenomenal PulmCrit post regarding this concept: https://emcrit.org/pulmcrit/submassive-pe-peitho/
C. Treatment of Submassive PEs
- For years the prevailing dogma is that in submassive PE, thrombolysis fixes the numbers but does nothing to improve clinically meaningful outcomes. The relatively low NNH due to ICH and other clinically significant extracranial bleeding was further evidence for skeptics that we really should not be doing this
- The heterogeneity of studies has muddled meta-analysis and yet still, the 2014 (somewhat controversial) Chaterjee paper found a mortality benefit to a preemptive thrombolysis approach in submassive patients, muted of course by the increased incidence of bleeding. It is important to note that that has never been an individual RCT that has shown a mortality benefit in lysing submassive patients
- In the view of experts, what is likely is that in acute, high risk submassive PE patients, thrombolysis may acutely drive the PA pressure down enough to prevent hemodynamic collapse and when done at a reduced dose (50mg/2hrs of tPA) likely does not confer a clinically increased risk of major bleeding
- The question of course is who are these patients who would benefit from lysis? This requires expertise and early consultation with your specialists. Some experts have advocated for the following patients to be closely examined for thrombolysis
Likely?
- Elevated shock index (HR/BP)
- Syncope or presyncope
- High Endogenous Stress
- Lactic acidosis
- Severely “ill appearing” or decompensating
Possibly?
- Severe hypoxemia
- Severe right ventricular dysfunction
- Extensive clot burden
The reason we lyse these patients is improvement of PA pressures just enough that it prevents hemodynamic compromise and a PEA arrest. The 2017 update to the PEITHO study quite convincingly shows that the long-term morbidity with regards to prevention of RV dysfunction and CTEPH, is likely not different, when compared to patients who were just anticoagulated.
D. Summary of Treatment Considerations (No Consensus and Must be Individualized!)
- Use a clinical decision rule to help guide your pre-test probability and management for suspected PE
- Attempt to identify high-risk submassive patients
- Obtain studies & interventions quickly with the early assistance of consultants (pulmonary, IR, cards)
- Thrombolysis in submassive patients should be restricted to patients at the greatest risk of death. In other words, it is likely most efficacious in acute, high risk submassive PE, not patients with stable subacute to chronic symptoms
- Reduced dose of thrombolytics are likely just as efficacious as the full dose, with clearly reduced risk of clinically significant and intracranial bleeding
- All of the above is not supported by any guidelines and for test question purposes, unless the patient is hypotensive, thrombolysis is probably not the right answer!
- Other Considerations
- Avoid volume loading an already dilated RV and if hypotensive, focus on norepinephrine
- Avoid intubation unless absolutely essential (attempt HFNC first if possible)
- iNO may have a role
