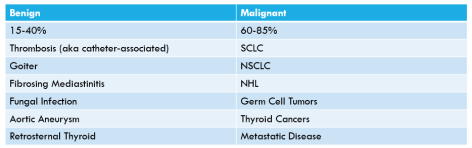
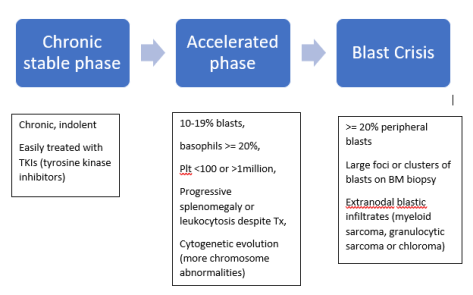
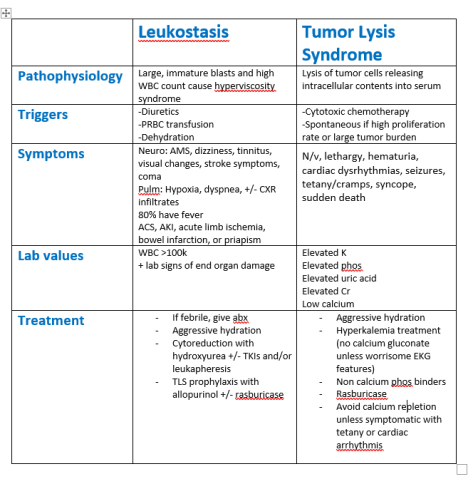
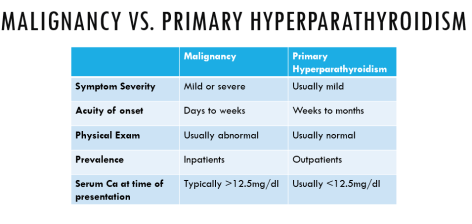
Today’s case was a young man with alcohol use disorder who presented with delirium tremens refractory to high dose benzodiazepines and severe anion gap metabolic acidosis.
In the differential diagnosis for hyperthermia, tachycardia, and hypertension in a patient with alcohol use disorder and psychiatric comorbidities, it is essential to consider serotonin syndrome and neuroleptic malignant syndrome in your differential.
| NMS | Serotonin Syndrome | DTs | |
| Onset | Gradual, days to weeks | <24h | 72-96h after last drink |
| Vital signs | Hyperthermia, tachycardia, labile or high BP | Hyperthermia, tachycardia, hypertension | Hyperthermia, tachycardia, hypertension |
| Neuromuscular | Muscle rigidity (lead pipe), hyporeflexia
|
Tremor, myoclonus, oculoclonus | Tremor |
| Reflexes | Hyporeflexia | Hyperreflexia | Hyperreflexia |
| Pupils | Normal | Mydriasis (dilated) | Mydriasis (dilated) |
| Causative agent | Dopamine antagonist | Serotonin agonists | Alcohol cessation |
| Treatment | bromocriptine | Benzos, cyproheptadine | Benzos |
| Resolution | Days to weeks | <24h | Variable |
The differential diagnosis for anion gap metabolic acidosis in an alcoholic patient is also wide, including alcoholic ketoacidosis, type A lactic acidosis from concurrent shock due to severe alcoholic pancreatitis, hepatitis, or aspiration pneumonia among other infections, type B lactic acidosis from ethanol itself, or coingestion of other toxic alcohols such as methanol or ethylene glycol.
It is important to rule out toxic coingestion in all patients with alcohol use disorder, altered mental status, and severe anion gap metabolic acidosis. Do this by calculating your serum osmolar gap with a formula that includes ethanol.
Serum osm= 2Na + BUN/2.8 + glucose/18 + ethanol/4.7
If the osmolar gap >10, coingestion should be high on your differential.