Today we discussed a case of a patient with chronic constipation who presented with abdominal pain and hematochezia. A CT scan revealed a large fecaloma, which led to stercoral ulceration of the rectum, colitis and eventually perforation.
We first reviewed the etiologies of hematochezia, remembering that in up to 15% of cases, a brisk UGI source is the etiology. When this occurs it is typically in patients who have hemodynamic instability. Some aspects to aid in the diagnosis were put together in an excellent Rational Clinical Examination article in JAMA that Dr. Jacobson referenced. Findings that have a high LR of a brisk UGI are melenic stool on examination, an elevated BUN/Cr ratio 30, an NG lavage with blood or CGE . Findings that have a high LR of the etiology being a LGIB is a history of LGIB and clots in stool.
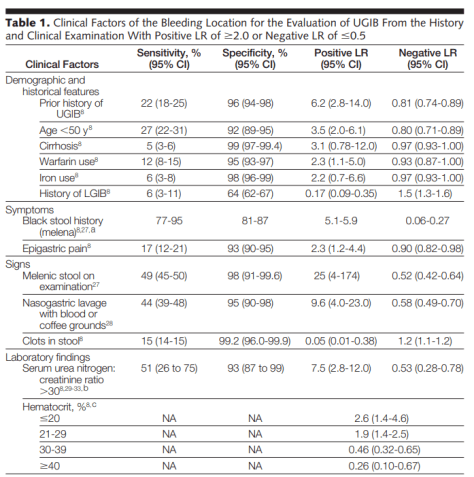
https://jamanetwork.com/journals/jama/fullarticle/1105075
We then discussed a framework for LGIB:

We discussed the complications of constipation:
- Decreased quality of life
- Hemorrhoids
- Anal Fissures/Tears
- Diverticulosis
- Rectal Prolpase
- Stercoral Ulceration
Stercoral Ulceration/Colitis/Perforation 101
- most cases have been reported in elderly, psychiatric, bedridden, or narcotic-dependent patients with a history of constipation
- Fewer than 150 causes of perforation have been described in the literature
- Severe chronic constipation thought to induce the formation of stone-hard fecalomas and maintain a continuous peressure over the bowel wall leading to pressure necrosis
- This ulceration sometimes leads to a state of stercoral colitis (localized ischemia due to increased luminal pressure)
- CT findings of perforation are fecal impaction, colonic dilatation, colonic wall thickening, discontinuity in the enhancement of the bowel wall in relation to focal fecal distension of the colonic lumen, and extraluminar free air
- A mortality rate of ~30% has been mentioned
- Treatment is generally surgical
