We discussed a case of a middle-aged man with uncontrolled diabetes, who presented with acute-subacute fevers, headache, L neck pain, L retroauricular pain, and was found to have L ophthalmoplegia, acute L eye swelling due to MRSA bacteremia, left skull base MRSA osteomyelitis, and septic cavernous sinus thrombosis.
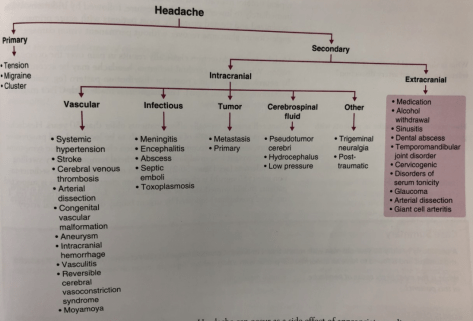
We reviewed various frameworks for secondary headache.
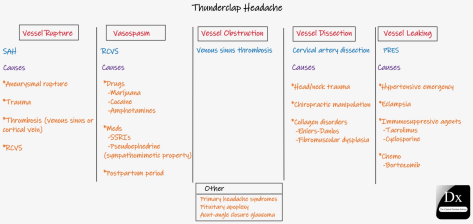
Thunderclap headache = Abrupt onset and reaches its max intensity within 1 minute or less of onset
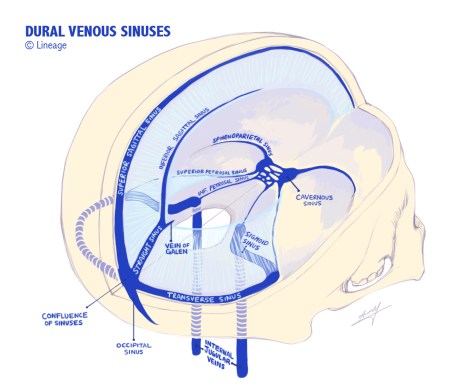
Cerebral venous thrombosis is a rare (1%) cause of strokes. It usually affects younger patients (20-50 y/o) with a female > male predominance.
In septic cerebral vein thrombosis, thrombosis most commonly arises from contiguous spread of infection (nasal, sinus, dental) into the veins/sinuses.
Risk factors for cerebral venous thrombosis include:
- Thrombophilia e.g. hx of prior VTE, oral contraceptives, obesity, pregnancy, autoimmune diseases (lupus, IBD, antiphospholipid), nephrotic syndrome
- Head and neck infections e.g. mastoiditis, sinusitis, otitis media, meningitis, cerebral abscess, Lemierre’s syndrome
- Mechanical causes e.g. trauma (at the skull base or jugular foramen), NSGY procedures, jugular vein procedures
Clinical manifestations to definitely watch out for include:
- Headache: acute to subacute, can be thunderclap headache
- Fevers
- Focal neuro symptoms: CN III, IV, VI palsies, paresis, dysarthria, diplopia…depending on where the clot is
- Seizure
- Encephalopathy
Treatment goals:
- Recanalize the occluded vein
- Prevent thrombus propagation
- Treat the underlying prothrombotic state
Treatment:
- Heparin (unfractionated or LMWH)
- Intracerebral hemorrhage is NOT a contraindication to anticoagulation.
References:
- CPS: secondary headache schema based on red flag symptoms
- CPS: thunderclap headache schema
- IBCC: cerebral venous thrombosis
- NEJM: septic cerebral venous thrombosis
- Uptodate: cerebral venous thrombosis – etiology, clinical features, and diagnosis
- Uptodate: cerebral venous thrombosis – treatment and prognosis
- Uptodate: septic dural sinus thrombosis