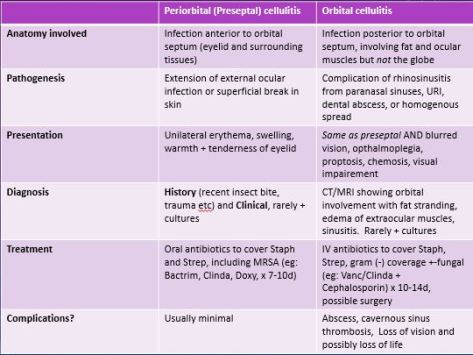
APML (Acute Promyelocytic Leukemia)–M3 variant of AML
Epidemiology
–ANY age but uncommon before age 10 or after age 60
-RF include exposure to cytotoxic chemotherapy or radiation (esp. Topoisomerase inhibitors)
Timing
-Sub-acute
S&S
-Related to pancytopenia (eg: pallor,fatigability, infections, gingival bleeding, ecchymoses etc.)
-APML in particular often presents with COAGULOPATHY due to DIC with Auer Rods seen on peripheral smear (see below)

How do you make the diagnosis?
Molecular genetics via FISH analysis most common method
-Most common translocation is T(15:17) creating the fusion gene PML-RARA (see image below)
-Can also use Karyotype, RT-PCR, or anti-PML antibodies.
–Bone Marrow Biopsy–if high suspicion for APML based on cytologic and clinical criteria, it is recommended to START treatment prior to BMB due to high rate of early mortality.

Treatment
-First line treatment is ATRA (All-Trans-Retinoic Acid)
- Combine with either Anthracycline based chemotherapy (Idarubicin or Daunorubicin and Cytarabine) or Arsenic Trioxide (ATO)
Which one do you choose?
- Low/Intermediate risk: ATRA + ATO– Lower risk of myelosuppression, cardiac toxicity, reduced risk of secondary leukemia
- High risk APL (Initial WBC count >10^9 and platelet<40): ATRA + Anthracycline*
90 % of patients will achieve hematologic complete remission (CR) with induction chemotherapy
Supportive Care
High risk of DIC and coagulopathy-Monitor DIC labs and transfuse to keep platelet count >20k-30k, and fibrinogen>150
Complications-ATRA Differentiation Syndrome
25 % of patients on ATRA may develop it within 2-25 days of treatment. However, can occur in those with APL who are NOT even treated with ATRA
Signs and Symptoms
-Fever, pulmonary infiltrates, peripheral edema, hypoxemia, AKI and pleural/pericardial effusion
-Looks like ARDS or sepsis
Treatment is with Dexamethasone (10 mg IV q12h x 3d) and often cessation of ATRA treatment.
References
Images and information from UpToDate