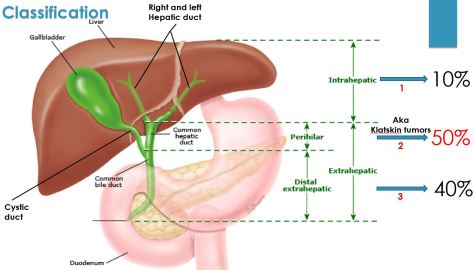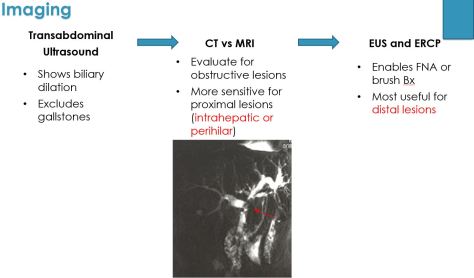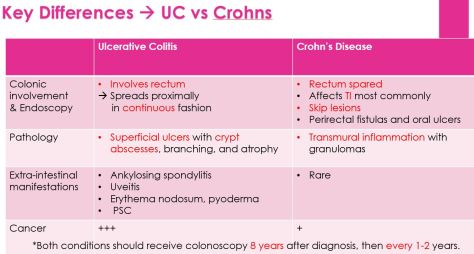












Labs will show:
Treatment
Consequences of ATRA
Platelet transfusion goals








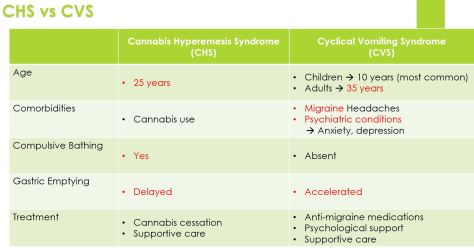









Most common etiologies of AS
Symptoms
Diagnosis
Low-flow, low-gradient AS
When to treat?
Treatment



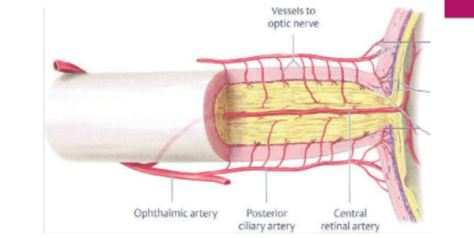


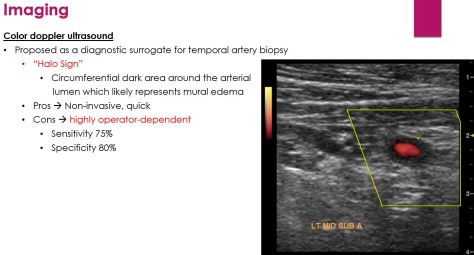



Mechanism of action:
Clinical features
Diagnostic tests
Treatment goals
Management
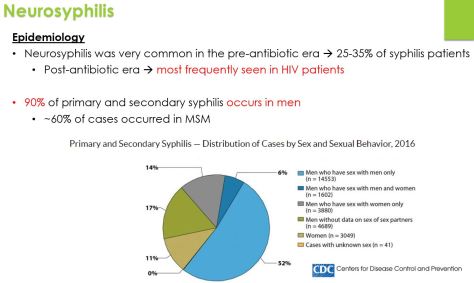

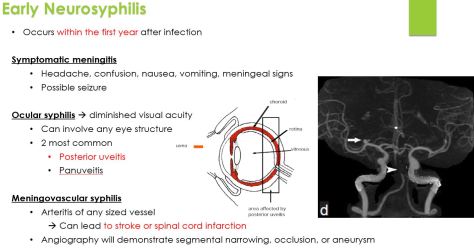








Remember that prolactin is inhibited by dopamine!
In panhypopituitaryism, the anterior pituitary hormones are more commonly affected than the posterior pituitary hormones and there is a spectrum for how much of the HPA axis is still preserved depending on the etiology of the panhypopituitaryism.
The hormones that need replacement in adults are T4 and cortisol. Testosterone can be replaced if needed in men. Estrogen and progesterone can be replaced in pre-menopausal women who do not want fertility at that time or in post-menopausal women to relieve post-menopausal symptoms. If a woman desires fertility and has enough HPA axis preserved then patients can get pulsatile GnRH to stimulate FSH and LH production to induce ovulation.
To screen for adrenal insufficiency, check a morning cortisol at 8am.
Stimulation tests
Adrenal crisis
Remember – if you suspect adrenal insufficiency, give stress dose steroids immediately without waiting for further testing!