- Thyrotoxic Periodic Paralysis is a channelopathy that causes intracellular shifts of potassium. Low serum potassium does not reflect a total body potassium deficit.
- Common triggers include: high-carb meals (insulin-mediated), stress (adrenergic state), intense exercise.
- Repletion of potassium should be gradual (~90mEq in 24 hrs) to prevent rebound hyperkalemia.
Tag Archives: Neurology
A Dizzying Topic
Today we discussed a case of a patient who had been reporting 6 months of “dizziness”. We first took a deep dive into dizziness and what exactly it means.
The single most important question to ask a patient with dizziness is: what do you mean by that?
Dizziness can then be classified into four major categories depending on the description of the symptoms (though of course this slightly antiquated framework does have limitations). We emphasized the importance of not coaching the patient to using certain descriptors and also recognized the cultural differences in the usage of the term dizziness (many communities utilize this word to indicate sickness, rather than how we define it).
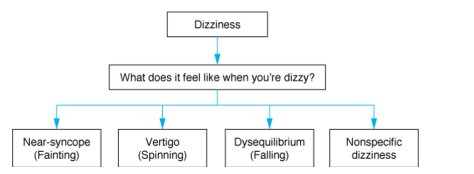
We focused our discussion on Vertigo as the patient reported a room-spinning sensation for the past 6 months. The major discussion is always central vs. peripheral vertigo and please see the excellent prior blog post discussing this in detail:
We reviewed some important distinguishing characteristics (as taken from a 2014 NEJM Review Article on BPPV)

The key takeaways are as follows:
1. BPPV is characterized by positional, brief (<1 minute) attacks of severe vertigo prompted by head movements and if nystagmus is seen, it is unidrectional. The typical discussion therefore is not BPPV vs a posterior CVA but rather an acute vestibular syndrome (vestibular neuritis/labrynthitis) vs. a posterior CVA.
2. If the Dix-Hallpike induces vertigo, this does not mean the patient has BPPV! The characteristics of the nystagmus however may be very helpful

3. The HiNTs exam can be exceptionally useful, but only in the right clinical context (it can only be used if the patient is currently symptomatic, and is meant for continuous, not intermittent, symptoms. (i.e hours – days)
- https://www.nuemblog.com/blog/hints
- Recognize the difficulty of performing the examination well (the initial study was done by one single neuro-opthalmologist and as far as we know, no inter-reliability study has been performed with a group of generalists
- Alarming findings are useful though and should prompt further investigation
- Remember, ALL three of the following components must be seen in order to state that the exam is truly negative (and therefore a peripheral vertigo)
- Unidirectional or no nystagmus
- No vertical skew
- Abnormal head impulse test (corrective saccade) – this indicates a nerve problem and therefore must be seen in order to state that the HiNTs exam is negative and therefore the vertigo is peripheral
4. Try not to overly rely on imaging, especially a head CT, which is at best, 16% sensitive for acute ischemia in the posterior fossa. Even MRI with DWI misses 15-20% of acute posterior fossa infarctions in the first 24 hours. Sensitivity for brainstem strokes is maximal 72-100 hrs after infarction
Heart-Stopping Syncope
Today we presented a case of syncope 2/2 to age-related degeneration of the conducting system leading to complete heart block. We first went through a framework for Syncope (taken from Dr. Eric Strong’s awesome lecture series)
Definition: Syncope is defined as a transient, self-limited loss of consciousness with an inability to maintain postural tone that is followed by spontaneous recovery.

Source: https://www.youtube.com/watch?v=iJ6g5rsQKaM&t=343s
We then emphasized the importance of choosing wisely in the workup of syncope. All patients with syncope should receive the following:
- A spectacular history
- A splendid physical examination
- An EKG
- Orthostatic vital signs
Depending on the above, target your further testing accordingly
Remember, it’s the cardiogenic syncope that is highly concerning and so the San Francisco Syncope Rule can be useful in deciding who is safe to discharge…BUT, as a recent paper reported, the sensitivity of clinical judgement for adverse outcomes secondary to a syncope is higher than decision making rules. Therefore, if something doesn’t feel right, trust your instincts!
Our patient was found to have complete heart block on an EKG and we reviewed the three major classifications for its etiology:
- Known Pathologic
- Ischemia
- Myocarditis (i.e lyme)
- Infiltrative cardiomyopathy (amyloidosis, sarcoidosis
- Iatrogenic
- Medication-related
- Post-cardiac surgery
- Post catheter ablation
- Post TAVR
- Idiopathic Progressive Cardiac Conduction Disease (>50% of cases)
- thought to be secondary to age-related degeneration of the conduction system
Finally, we discussed management of complete heart block:
- Atropine use should be avoided since it is likely ineffective (since the block is likely below the AV node) and more importantly it delays more effective treatment
- Electrical & Medication options (either epinephrine OR dopamine) should be considered
- Unless the cause is immediately reversible, patients will generally need a transvenous pacemaker and then a permanent pacemaker
If you made it this far in the post, congratulations. As a reward, do note that the framework for syncope actually has a mnemonic embedded within it (ROCS) 🙂
Journal Club!
Quick rundown of the articles we talked about today in morning report:
- ANDROMEDA-SHOCK trial, JAMA 2019: RCT of 424 patients with septic shock randomized to capillary refill vs lactate to target resuscitation efforts. Primary outcome of interest was 28 day mortality. While the difference between the two groups was not statistically significant, the study may have been underpowered. Interestingly, there were lower rates of organ dysfunction at 72 hours with the cap refill guided resuscitation than lactate. So keep doing your cap refill bedside exam!
- E-cigarettes vs nicotine-replacement therapy (NRT): Multi-center RCT in the UK that randomized 886 people to e-cigarettes or NRT of their choice for 3 months. Outcome of interest was abstinence from smoking at 6 months and 1 year. They found a significantly higher rate of abstinence in the e-cigarette group than the NRT group. However, while only 9% of the abstinent NRT users were still using NRTs at 1 year, over 80% of the abstinent e-cigarette users were still using e-cigarettes at the end of the study period! Together with the alarmingly high incidence of e-cigarette use amongst adolescents, the results of this study would have to be interpreted cautiously.
- EAGLES trial. Lancet. 2016: Multi-center, double-blind, RCT looking at neuropsychiatric effects of varenicline (Chantix), bupropion, or nicotine patch or placebo involving ~4k people without psych history and 4k people with psychiatric history. Study found that Chantix resulted in the highest rates of sustained abstinence across all study arms. In the psychiatric cohort, there were no differences between the treatment groups in terms of rates of psychiatric events. Bottom line: use Chantix whenever you can to help your patients trying to quit smoking!
- EXTEND trial. NEJM. 2019: Multi-center, randomized, placebo-controlled trial of 225 patients who presented with ischemic stroke within 4.5-9 hours after onset of symptoms with radiologic evidence of salvageable brain tissue randomized to receive tPA vs conservative management. The primary outcome of interest was functional status at 90 days and was significantly better for the intervention group vs control arm. Caveats are that symptomatic intracranial hemorrhage was six times higher in the intervention group than the control arm. 65% of the patients in the study woke up with neurologic deficits and had an unknown time of onset.
- Thyroid hormone replacement for subclinical hypothyroidism (Feller et al. JAMA. 2018): Meta-analysis of 21 RCTs with 2192 patients randomized to hormone replacement or no replacement. The study found no significant difference in qualify of life, thyroid replacement symptoms, fatigure/tiredness, depression, cognition, or SBP after 12 months of therapy. Based on this study, the new guidelines state that in patients with no symptoms of hypothyroidism or non-specific symptoms of hypothyroidism who have fT4 within normal limits and TSH <20, thyroid hormone therapy is strongly recommended against.
Monthly Journal Club 4/30/2019
We see patients with ischemic strokes pretty frequently as Internists. We will use today’s journal club to go over some basics of acute ischemic stroke management, and the studies behind our management.
We went over CHANCE, POINT, SPARCL, FLAME, and FOCUS in detail, but the hyperlink to the other trials we briefly mentioned are included!
Acute Stroke Management
- ABC: Airway, breathing circulation
- History, physical, glucose, O2 sat, EKG, noncon head CT ASAP
- Determining time last see normal to see if patient is a candidate for tPA
- 3-4.5 hours
- Mechanical thrombectomy can be considered 16-24 hours (DAWN, DEFUSE 3)
- Additional studies as needed depending on pre-test probability
- TTE, carotid US, etc if needed
- Things to consider in the acute setting
- Fluids:
- Ensure euvolemic, hypovolemic esp in older adults can worsen cerebral blood flow.
- Hypoglycemia:
- Severe hypoglycemia can cause neuronal injury, rapidly correct any hypoglycemic state
- Hyperglycemia:
- Associated with poor outcome in stroke patients. AHA/ASA guidelines aim for BG 140-180mg/dL
- SHINE trial: tight glycemic control vs standard of care, no different in outcome
- Swallow: Dysphagia screen prior to giving oral meds or food, aspiration precautions.
- Head and body position:
- Elevated head of the bed to 30 degrees if concerned for elevated intracranial pressure like is ICH, cerebral edema from large ischemic infarction, aspiration, or cardiac/pulm disease
- Mobilization:
- Do so after 24 hours after, dec risk of PNA, DVT, PE, pressure sores. Very early < 24 hours mobilization is associated with dec favorable outcome at 3 months (AVERT trial)
- Fever:
- Rule out infectious etiology
- Can be present after brain injury, fever within 24 hours is associated with 2x inc in mortality at one month.
- Blood pressure
- Ischemic stroke only
- Stabilize blood pressure below 180/105 for at least 24 hours if s/p tPA
- If no tPA, permissive HTN, do not treat the BP unless SBP > 220 or DBP > 120, or if pt has underlying CAD, HF, aortic dissection, hypertensive emergency.
- Lower BP by no more than 15% in the first 24 hours
- Rate of blood pressure control will be dependent on vascular imaging, if a large artery stenosis is found, keep BP high to maintain cerebral blood flow.
- Choice of meds: IV preferred, titratable, precise
- Labetalol
- Nicardipine
- 2nd line: Nitroprusside, inc risk of inc ICP, inc risk of stroke in older folks
- Secondary prevention
- Ischemic stroke only
- Fluids:
DAPT After Stroke
- CHANCE
- Population
- 5170 Chinese patients with high risk TIA or minor ischemic stroke within 24 hours of sx onset
- Intervention
- Combination ASA/Plavix x 21 days, then aspirin
- Comparison
- Aspirin alone
- Outcome
- 90 day subsequent strokes
- DAPT associated with 3.5% absolute reduction (8.2% vs 11.7%), NNT 29
- No difference in bleeding events
- 90 day subsequent strokes
- Comment
- Main criticism: Chinese patients have a larger proportion of undertreated modifiable stroke risk factors i.e. DM and HTN and greater burden of large vessel cerebrovascular disease. Also Chinese population might have polymorphisms in genes regulating Plavix metabolism.
- How to apply to US population?
- Population
- POINT
- Population
- 4881 US patients within 12 hours of a minor strokes or TIA
- Intervention
- 90 days DAPT and then aspirin
- Comparison
- Aspirin monotherapy
- Outcome
- Ischemic stroke: Absolute risk reduction of 1.5% in the DAPT group
- Bleeding: Absolute risk increase of 0.5%, NNH 200
- Comment
- Generalizable to US population
- 90 day DAPT vs 21 in CHANCE!
- Ongoing THALES trial looking at 30-day, but aspirin/ticagrelor vs aspirin
- Population
Statins
- SPARCL
- Population
- 4731 patients with prior stroke or TIA
- Intervention
- High intensity statin (atorvastatin 80mg daily)
- Comparison
- Placebo
- Outcome
- Fatal/non-fatal stroke occurrence at 5 years
- HI Statin group reduced composite primary outcome of fatal or non-fatal stroke at 5 years
- Overall a 2.2% absolute risk reduction, NNT to prevent one stroke at 5 years is 45.
- Comment
- Industry funded
- Later analyses revealed associated with HI Statin with hemorrhagic stroke
- Excluded: Non-ambulatory, AF, cardiac emboli, SAH, high LDL > 160 in some centers
- Population
Antidepressants?
- FLAME (Lancet 2011): Does early administration of fluoxetine in addition to standard therapy improve recovery after an ischemic CVA?
- Population
- 113 patients after acute stroke, randomized to early fluoxetine or placebo
- Intervention
- Addition of fluoxetine to post stroke secondary prevention 5-10 days after event
- Comparison
- Placebo
- Outcome
- 90 day FMMS Scores (measurement of motor recovery)
- Intervention group has better outcome vs the control group on the FMMS (P = 0.003)
- 90 day FMMS Scores (measurement of motor recovery)
- Comment
- Small sample size
- Short follow up
- Population
- FOCUS (Lancet 2018)
- Population
- 3127 patients after acute stroke (2-15 days after), mostly ischemic stroke.
- Intervention
- Fluoxetine in addition to standard therapy
- Comparison
- Placebo
- Outcome
- Modified Rankin Scale Scores (mRS) at 6 months
- No difference between the 2 groups
- Fluoxetine group has lower rate of depression than placebo (13% vs 17%) but higher rates of bone fractures (2.9% vs 1.5%)
- Comment
- Better designed and powered, no benefit in terms of stroke recovery but associated with inc harm.
- AFFINITY Trial in Australia ongoing, also investigating the use of early SSRI in post-stroke care.
- Population
Crowned Dens Syndrome!
Thanks to Eric and Naina for presenting the fascinating case of an elderly man who presented to the ER with acute, progressive shoulder and neck pain/stiffness that started after a visit to the dentist, found to have Crowned Dens Syndrome (???!!!) on CT imaging!
Clinical Pearls
- The exam maneuvers we use to determine nuchal rigidity (neck stiffness, Kernig, Brudzinski signs) are not sensitive for meningitis. Kernig and Brudzinski, when present, are highly specific. Jolt accentuation is more useful as a screening tool because it is highly sensitive (>90%) but not very specific (~60%).
- Make sure to check out Beers list when prescribing new meds for our geriatric patients.
- For patients presenting with traumatic neck pain, consider using NEXUS or Canadian C spine rules to help you determine whether CT imaging is necessary.
- Crowned Dens Syndrome is a rare finding in patients with CPPD and refers to deposition of calcium pyrophosphate crystals in and around the atlanto-axial articulation, which resembles a crown on CT imaging (image here).
- The knee accounts for 50% of all acute CPPD flares.
Nexus criteria
- No indication for CT if all of the following criteria are met
- Absence of posterior cervical spine tenderness
- Normal level of alertness
- No evidence of intoxication
- No abnormal neurologic findings
- No painful distracting injuries
Canadian C-spine Rule
- Step 1: CT indicated if any of the following are present:
- Age > 65 years
- Dangerous mechanism of injury
- Paresthesias in the extremities
- Step 2: Assess for low risk factors that allow for safe examination of the cervical spine range of motion
- Simple rear-end mechanism
- Sitting position in the ED
- Ambulatory at any time
- Delayed onset of neck pain
- Absence of midline cervical spine tenderness
- If ALL of these are present proceed to step 3
- Step 3: Examine range of motion
- Test active range of motion
- Perform radiography in patients who are not able to rotate their neck actively 45 degrees both left and right. Patients able to rotate their neck, regardless of pain, do not require imaging
CPPD:
- Umbrella term that covers
- Pseudogout: acute synovitis/flare
- Chondrocalcinosis: radiographic calcification in hyaline and/or fibrocartilage
- Pyrophosphate arthropathy
- Epi
- 4-7% of adults
- ~50% of those with radiographic findings are >84 years of age
- Clinical manifestations
- Asymptomatic (majority)
- Acute CPP crystal arthritis: self limited acute or subacute attacks of arthritis involving one or several extremity joints. Knee is affected in over 50% of all acute attacks followed by wrists, shoulders, ankles, feet, and elbows.
- Triggers: Trauma, surgery, severe medical illness. Abnormalities in serum calcium, magnesium, bisphosphonates, hemochromatosis.
- Chronic CPP arthritis
- Chronic inflammatory arthritis (5% of cases): resembles RA, multiple joints involved
- Chronic osteoarthritis: Most prevalent form of symptomatic disease.
- Severe joint degeneration
- Spinal involvement
- Crowned dens syndrome: rare, characterized by severe acute or recurrent axial neck pain, neck and shoulder girdle stiffness, and associated fever, elevated inflammatory markers, and CPP or calcium phosphate crystal deposition on CT in and around the atlanto-axial articulation
- DDx would include PMR, Milwaukee shoulder (deposition of hydroxyapatite crystals, commonly seen in women >70 years of age) less frequently meningitis, cervical discitis, or inflammatory spondyloarthritis
- Favorable response to NSAIDs and colchicine
- Crowned dens syndrome: rare, characterized by severe acute or recurrent axial neck pain, neck and shoulder girdle stiffness, and associated fever, elevated inflammatory markers, and CPP or calcium phosphate crystal deposition on CT in and around the atlanto-axial articulation
Pituitary Apoplexy 4/8/2019
Thanks Brandan for presenting an elderly lady who developed sudden onset headache, CN3 palsy, and bitemporal hemianopia. She had a CTH that was unremarkable the day before, and a repeat CT found a large pituitary “mass,” and MRI was concerning for pituitary apoplexy!
This case demonstrates a few important concepts:
Visual Field Pathology (commonly tested!)
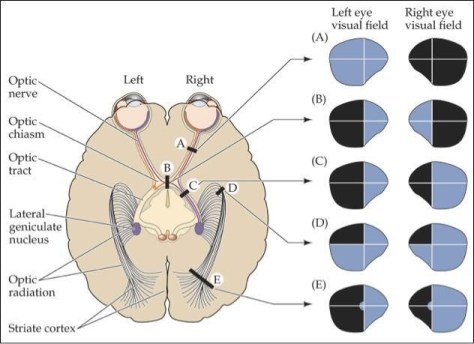
A: Optic Nerve pathology or structural pathology leading to complete blindness in one eye, i.e. trauma, optic nerve neuropathy, optic neuritis (i.e. MS)
B: Bitemporal hemianopsia= optic chiasma pathology until proven otherwise.
C: Homonymous hemianopsia: Optic tract pathology
D: Homonymous quadrantanopsia: Optic radiation, think occipital lobe pathology
Oculomotor nerve palsy (CNIII palsy)
- Findings: Down and out on the affected eye.
- Physiology: Lacteral rectus, with CN VI innervation, remains intact and not opposed by the medial rectus which is innerved by CN III. Down because the superior oblique (innerved by CN IV) is unopposed by the paralyzed superior rectus, inferior rectus, and inferior oblique
- DDx:
- Ischemic (affects somatic fibers over parasympathetic, typically spares the pupils)
- Inflammation,
- Infection
- Tumors (mass effect so both somatic and parasympathetic fibers are typically affected)
- Demyelinating disease
- Autoimmune
- Cavernous sinus thrombosis (don’t miss this!)
Pituitary apoplexy: A Medical Emergency!
- Pathophysiology:
- Hemorrhage or infarction of the pituitary gland usually involving a pituitary adenoma, and occasionally it may be the first manifestation of a pituitary adenoma.
- Risk factors:
- HTN, surgeries, coagulopathies, certain meds (i.e. VKA, DOACs, antiplatelets)
- Presentation:
- Sudden onset headache, vomiting, encephalopathy, visual field defect, hemodynamic instability (esp with ACTH defects).
- DI is very common in the immediate setting, but as axons in the pituitary die, ADH is released which can lead to SIADH (but only transient until stores of ADH are used up), followed by recovery but it depends on the extent of the damage.
- Management: IVF, hydrocortisone (get labs first)
- Acute secondary adrenal insufficiency is seen in 2/3 of pts, important cause of mortality.
- Acute hypocortisolemia leads to hemodynamic instability
- Inc vasopressin release from posterior pit can lead to fluid and lyte disturbances.
- Any signs of hemodynamic instability: Can do 50-100mg hydrocortisone Q6H or continuous infusion 2-4mg/hr
- Role of surgical management:
- Decision to operate based on whether there is deteriorating level of consciousness, severely reduced visual acuity, or presence of visual field defects.
- Otherwise, medical management with corticosteroids, monitoring, re-evaluation is recommended.
- Vision outcomes: Conflicting data on medical vs surgical management.
- Pituitary function outcomes: No difference b/w surgical vs medical management
- Acute secondary adrenal insufficiency is seen in 2/3 of pts, important cause of mortality.
Please refer to this paper for a detailed read on pituitary apoplexy!
Wernicke’s Encephalopathy in Setting of Hyperemesis Gravidarum and Unexpected Pregnancy! 4/4/2019
Credit goes to Dr. Jon Reitzenstein from Michigan State!
Today we went over a case featured on the Human Diagnosis Project.
A 28yo F with no medical history presents with 1 day history of unsteady gait, with associated “indifference” per her husband and intermittent diplopia. She also has been having significant N/V for the past 3-4 weeks, barely able to keep anything down. She was dehydrated on exam with elevated spec grav and ketones on the UA. Her pregnancy test returned positive (estimated 6 week old fetus). Ultimately she was given thiamine with rapid symptomatic improvement.
The final diagnosis is Wernicke’s Encephalopathy in setting of poor nutritional intake and increased metabolic demands secondary to unexpected/unknown pregnancy.
Wernicke’s Encephalopathy
Epidemiology
- Most cases are associated with chronic EtOH use but not all the time!
- Non-alcohol related:
- Hyperemesis gravidarum
- Bariatric surgery
- Long-term TPN
- HIV
- Malignancies
- Extreme poverty, war zones, refugees
- More common in men
- Up to 12.5% of pts with chronic EtOH
Pathophysiology
- Chronic inadequate intake of thiamine (vitamin B1) leading to degeneration of the peripheral nerves, thalamus, mammillary bodies, and cerebellum.
Presentation: triad of
- Encephalopathy (disorientation, inattentiveness, indifference)
- Gait ataxia
- Oculomotor symptoms (nystagmus, lateral rectus palsy, conjugate gaze palsies)
- Triad only seen in 1/3 of patients, most only have around 2.
- Other signs: Memory impairment, hypothermia, electrolyte derangements often related to dietary, withdrawal if related to alcohol
Diagnosis: Clinical but there is a proposed Caine Criteria, 2/4 of these meet Caine Criteria for Wernicke encephalopathy. Sensitivity up to 85%
- Dietary deficiency
- Oculomotor abnrl
- Cerebellar dysfunction
- Encephalopathy or memory impairment.
- Serum thiamine is rarely tested and takes a while to come back, so when in doubt, start thiamine and don’t wait for levels.
- MRI might show hyperintensities around the periaqueductal white matter and thalami
Management
- Always give thiamine first and NOT glucose.
- Thiamine must be repleted first or else glucose infusions may worsen symptoms.
- Alcoholics should receive IV thiamine, at least 100mg, before receiving any IV glucose solutions.
- Thiamine:
- 500mg IV TID x 3 days, then 250mg IV daily for 3-5 days, then transition to 100mg PO daily.
Prognosis
- Prompt thiamine treatment leads to improvement in ocular sx within hours to days.
- Vestibular/gait improves within weeks.
- 60% will have residual ocular symptoms and gait abnormalities. Up to 80% of patients might have residual memory deficits.
Korsakoff Syndrome: Irreversible. Memory loss (selective anterograde or retrograde amnesia), confabulation, +/- hallucinations
Hyperemesis Gravidarum
Presentation
- Uncontrollable vomiting during pregnancy that results in dehydration, weight loss, and ketosis.
- Usually begins at about 5 weeks of gestation, peaks at 9 weeks, and resolves by 16-18.
- While vomiting in pregnancy (esp in the morning) is common, HG is an extreme form.
Diagnosis: Clinical, laboratory abnormalities
Management: Supportive, antiemetics
- Doxylamine + Vit B6
- Promethazine (Phenergan)
- Metoclopramide (Reglan)
- Ondansetron (Zofran)
- Prochlorperazine
- Corticosteroids (methylprednisolone) can be trialed if initial treatment is ineffective. Generally avoided prior to 6 weeks of gestation (organogenesis)
Severe Metabolic Acidosis Secondary to… Methanol Poisoning 4/3/2019
Credit goes to Eric for informing us about this case!
A 48yo M presents with acute onset encephalopathy. He has a distant history of alcohol abuse, and during the day of presentation he had complained about not being able to see. On presentation, his labs were notable for an anion gap of 35 with bicarb of 4, lactic acid of 11.9, ABG of 6.56/52/336, and osm gap of 65. Volatile screen ultimately came back positive for methanol level of 145.56 mg/dL (yes this is very high). He was given bicarb pushes, fomepizole, and urgent dialyzed.
It turns out that he might have ingested Klean Strip denatured alcohol, which is 40-60% methanol!
Methanol Toxicity
Pathophysiology
- Toxic metabolite of methanol poisoning is formic acid, which is formed from formic acid after methanol is metabolized in the liver by alcohol dehydrogenase and aldehyde dehydrogenase
- Leads to retinal injury and eventual blindness (permanent)
- Formic acid can also cause ischemic or hemorrhagic injury to the basal ganglia, hence in methanol poisoning you might see changes around the area (putamen is part of the basal ganglia).
- Ingestion of 1g/kg is fatal, and toxicity has been reported in as little as one teaspoon
- Ethylene glycol, on the other hand, mainly causes renal damage. (Flank pain, hematuria, oliguria). Buzz words = calcium oxalate crystals in urine.

Presentation
- Visual blurring, central scotomata (black spot in center of vision), and blindness are suggestive of methanol poisoning.
- Eye exam might reveal: mydriasis, retinal edema, hyperemia of the optic disk
- Co-ingestion of ethanol can delay presentation of toxicity.
- Labs:
- Profound AGMA, bicarb often < 8 mEqL
- High serum lactate
- Elevated plasma osmo gap
- Calculated osmolality = 2 x [Na mmol/L] + [glucose mg/dL] / 18 + [BUN mg/dL] / 2.8 + [Ethanol/3.7]
- OG = Measured osmo – calculated osmo
- Nrl < 10
- Typical agents that inc the osmolar gap:
- Methanol
- Ethylene Glycol
- Diuretics (osmotic diuretics i.e. mannitol)
- Isopropyl alcohol
- Ethanol
- Osmo gap takes Into account the quantity of uncharged molecules, hence it will only be elevated in presence of the parent alcohols.
- In late presentation: most alcohols have been metabolized already into charged active metabolic, hence osmo gap is not very sensitive in late presentation.
Management
- ABC comes first.
- Sodium bicarb administration
- Corrects systemic acidosis, which limits penetration of formic acid by converting it into negatively charged formate, which cannot cross cell membrane to cause damage.
- Formic Acid <- -> H+ & Formate-, adding bicarb dec H+, hence driving the equilibrium equation to the right. See? College O-chem is still helpful.
- HCO3 (mEq) required = 0.5 x weight (kg) x [24 – serum HCO3 (mEq/L)], and in general up front give 1-2 mEq/kg via IV bolus for any patients with pH < 7.3 followed by a sodium bicarb D5 gtt, at least 150-250cc/hr to correct acidosis
- Goal of infusion is to keep pH above 7.35
- Bicarb can be found in:
- Most common: 8.4%, 1mEq/mL, 1Amp = 50mEq, you will see these in the crash cart, very helpful to familiarize yourself with setting the syringe up for injection in a code blue situation!
- Gtt: 100-150 mEq/1000 mL in D5
- Concentrated gtt: 1mEq/mL, might need pharmacy’s help in formulating this. You can only use this in the ICU!
- PO tabs: Useful for CKD patients
- Corrects systemic acidosis, which limits penetration of formic acid by converting it into negatively charged formate, which cannot cross cell membrane to cause damage.
- Inhibition of alcohol dehydrogenase in the liver
- Fomepizole
- 1st line
- Loading: 15mg/kg, followed by 10mg/kg Q12hr, continue until blood pH is normalized and serum methanol is less than 20mg/dL
- Ethanol: ADH has better affinity for ethanol, leading to competitive inhibition.
- Difficult to dose, sedating effect, cannot be used in cirrhosis patients, pregnant patients.
- Fomepizole
- HD indicated if:
- Severe acid-base derangements, or even high AGMA regardless of drug level
- Severe levels of methanol
- End organ damage
- Interacts with fomepizole, hence if concurrent therapy, fomepizole should be dosed Q4H
- Co-factor therapy
- All methanol patients treated with ADH inhibition should also receive:
- Leucovorin 50mg IV (folinic acid) or folic acid Q6H
- Thiamine also commonly administered due to unclear nutritional status.
- All methanol patients treated with ADH inhibition should also receive:
- GI decontamination: Has no role whatsoever.
Leprosy!
Today, we talked about the case of a middle-aged man from the Philippines who presented with a one year progressive pruritic rash involving the face, arms, and legs as well as a distal symmetric peripheral neuropathy, found to have lepromatous leprosy on skin biopsy!
Clinical Pearls
- Mycobacterium leprae and lepromatosis like to grow in cooler areas, so infection often manifests in the skin and the peripheral nerves.
- Transmission is likely via respiratory route, through broken skin, and by touching armadillos!
- Early recognition and treatment is important to prevent injury to peripheral nerves.
DDx for rash + neuropathy
- Lyme (usually cranial nerves, radiculopathy)
- Celiac
- Zoster (tends to be painful rather than pruritic and localized to a dermatome)
- WNV (flaccid paralysis)
- Sarcoid
- Amyloid
- Syphilis
- Leprosy
Our patient presented with a pruritic rash and largely a distal symmetric peripheral neuropathy. We generated the following Venn diagram in report to help us with the diagnosis:

Leprosy
- AKA Hansen’s disease
- Infection caused by mycobacterium leprae and mycobacterium lepromatosis, separate species that cause similar clinical disease. They are both obligate intracellular parasites.
- Involves the skin and peripheral nerves
- Early treatment is important to prevent involvement of the eyes, hands, and feet due to neuropathy. The neuropathy is often non-reversible.
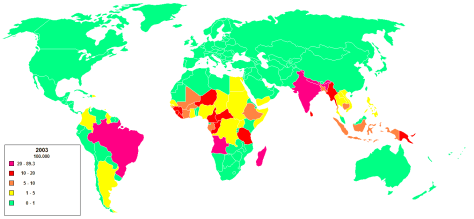
- 205 new cases detected in the US in 2010. 75% among immigrants (most commonly India, Brazil, Indonesia, Bangladesh, and Nigeria)
Transmission
- Unknown but probably respiratory route especially in lepromatous leprosy. Sometimes can transmit through broken skin. Also from armadillos.
- Most people do NOT develop disease after exposure. Risk factor for disease development include older age, genetic influences, and immunosuppression.
- Grows in cooler areas
Clinical presentation:
- Described in categories pertaining to how much bacillary burden of disease is present with tuberculoid being the least amount and lepromatous having the highest disease burden.
- Clinical features:
- Hypopigmented or reddish patches on the skin
- Typically involve the earlobes with nodular thickening and distributed symmetrically on the body in lepromatous leprosy.
- Diminished sensation or loss of sensation within skin patches
- Paresthesias of hands/feet
- Neuropathy occurs early in disease course
- Painless wounds or burns on the hands or feet
- Lumps or swelling on the earlobes or face
- Tender, enlarged peripheral nerves
- Hypopigmented or reddish patches on the skin
- Late findings in disease course:
- Weakness of the hands with claw fingers, foot drop, facial paralysis, lagophthalmos (can’t close eyes completely due to CN7 palsy), lack of eyebrows/eyelashes, collapsed nose, perforated nasal septum.
- Intermittent bacteremia can lead to focal lesions in various organs (liver, bone marrow, testicles and larynx)
Diagnosis:
- Consider it in patients with skin lesions and/or enlarged nerve(s) accompanied by sensory loss.
- No reliable blood or skin tests available.
- Usually clinical and skin biopsy
Treatment:
- Goal: Prevent and/or minimize injury to peripheral nerves!
- Often times it’s loss of sensation but later can progress to painful neuropathy
- Dapsone plus rifampin for tuberculoid leprosy. Clofazimine is added for lepromatous leprosy.
- Duration can be up to 24 months
- Treat neuritis with steroids for a prolonged course
- Make sure to screen for G6PD deficiency before prescribing dapsone
- Monitor liver function with rifampin
- Clofazimine (causes phototoxicity) is not available in US pharmacies and must be obtained from the NHDP.
Prognosis:
- May take a few years for skin lesions to resolve completely with treatment
- Very curable, low relapse rates, typically no drug resistance