A 42yo homeless man with AIDS not on ART with CD4 < 10, VL 440K+, presents with an acutely enlarging right-sided neck mass that was tender and firm, with associated fevers and malaise… Blood CrAg returned positive, and biopsy revealed encapsulated yeast with narrow based buds…
Yep, you’ve guessed it, it’s crypto!
Cryptococcus
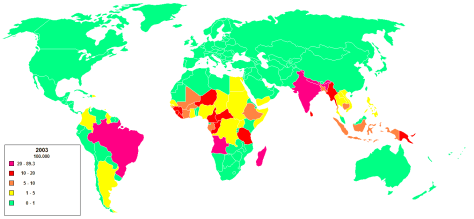
Epidemiology
- Invasive fungal species, primarily C neoformans and C. gattii are seen, found world wide in soil. Associated with infections in immunocompromised hosts.
Risk Factors
- AIDS (AIDS defining illness)
- Hematologic malignancies
- Long term steroids
- Solid organ transplantation
- Sarcoidosis
Presentation
- Most of the population have been exposed to the spores of C. neoformans, and in immunocompetent patients, most cases are asymptomatic to mild symptoms.
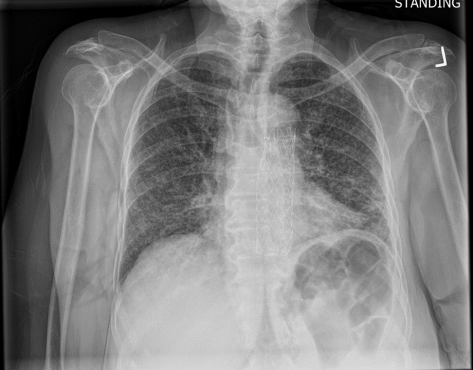
- Typically inhaled and affects the lungs first, and then can disseminate to CNS (most feared), skin, solid organs, bones, etc
- CNS: Feared, no-specific sx of fever, AMS, headache.
- Disseminated disease requires at least 2 non-contiguous sites
Diagnosis
- Culture is definitive
- GS: Encapsulated budding yeasts with narrow based buds on India Ink = characteristic
- IF e/o dissemination, get CXR, urine, LP, blood cultures
- Cryptococcal capsular antigen (CSF or blood) are > 90% sensitive and specific.
- Cr titers correlate with organism burden and prognosis, but not helpful to follow during treatment and doesn’t correlate with tx response. Titers > 1:512 is associated with poor prognosis.
- CSF or blood CrAg is diagnostic
Management
- Mild to moderate in immunocompetent hosts: Fluconazole for 6-12 months.
- Alternatives are itraconazole, voriconazole, or posaconazole.
- Immunocompromised hosts with mild-moderate pulmonary disease in the absence of diffused pulm infiltrates, CNS, or disseminated infection, can use fluconazole 6mg/kg (typically 400mg) daily for 6-12 months, with similar alternatives if fluconazole is not available/tolerated.
- Immunocompromised hosts with severe disease or CNS infection: ARDS occur frequent in IC patients with cryptococcal pneumonia.
- Induction: Ampho B + flucyotosine for minimum of 2 weeks.
- Consolidation: Fluconazole 200-400mg daily x 8 weeks
- Maintenance therapy is continued for at least 1 year.
- Intracranial pressure control: Cryptococcal meningoencephalitis patients might need daily LPs to relief ICP, might require VP shunt. Do not use mannitol or acetazolamide.
- Steroids not shown to be helpful.
- ART: Usually not started with induction therapy due to a risk of IRIS.
- ART is usually started 2-10 weeks after antifungal therapy has been started to minimize risk.