Today, Michael presented the case of a young woman with history of Sickle Cell Disease who presented with acute onset of CP, SOB, and pain, found to have new opacities on chest imaging and fevers concerning for Acute Chest Syndrome (ACS) with worsening symptoms requiring transfer for exchange transfusion.
Clinical Pearls
- Leading cause of death in patients with SCD is acute chest syndrome (ACS)
- ACS is defined as new radio density on chest imaging with fevers and/or respiratory symptoms.
- Most common causes of ACS are bone marrow/fat embolism and CAP
- There is no clinical/laboratory standard for diagnosing acute sickle cell crisis.
- Hydroxyurea can decrease crisis frequency, ACS events, need for transfusions, hospitalizations, and death.
DDx of liver injury in the setting of SCD
- Gallstones
- Hepatic sequestration
- Viral hepatitis
- Iron overload from transfusions
- Sickle cell intrahepatic cholestasis
Acute SCD complications
- Infections
- Severe anemia (due to splenic sequestration, aplastic crisis, or hyperhemolysis)
- Vaso-occlusive phenomena
- Pain
- Stroke
- ACS
- Renal infarction or med toxicity
- Dactylitis/bone infarction
- MI
- Priapism
- VTE
Acute chest syndrome
- Defined as a new radio density on chest imaging with fever (38.5) and/or respiratory symptoms
- >2% decrease in SpO2 from a documented steady-state value on room air
- PaO2<60 mmHg
- Tahcypnea
- Use of accessory muscles of respiration
- Chest pain
- Cough
- Wheezing
- Rales
- Leading cause of death for patients with SC disease
- Etiology of ACS in adults is commonly due to bone marrow or fat emboli followed by PNA
- 50% of patients with SCD will have an episode of ACS
- 80% of ACS episodes are associated with a vaso-occlusive pain episode
- Morality rate is 4.3%
- Clinical approach
- Determine severity (affects treatment)
- Mild
- SpO2 >90% on RA
- 1 lobe affected by infiltrates
- Moderate
- SpO2 >85%
- 2 lobes affected
- Severe
- Respiratory failure à mechanical ventilation
- 3 lobes affected
- Treatment
- Acute episode
- Pain control
- IVF (prevent hypovolemia but also avoid volume overload because it can worsen ACS)
- Blood transfusion:
- Mild ⇒ no transfusion
- Moderate ⇒ simple transfusion
- Severe ⇒ exchange transfusion (Goal Hg =10, HgS <30%)
- Antibiotics
- For CAP and atypicals x 7 days
- Supplementary O2
- Incentive spirometry
- DVT ppx
- Prevention
- Hydroxyurea (decreased incidence of ACS by 50%)
- Not good for acute episode
- Chronic transfusion therapy
- For those with > 2 episodes of moderate to severe ACS in 24 months despite hydroxyurea therapy
- Hydroxyurea (decreased incidence of ACS by 50%)
- Acute episode
- Mild
- Determine severity (affects treatment)

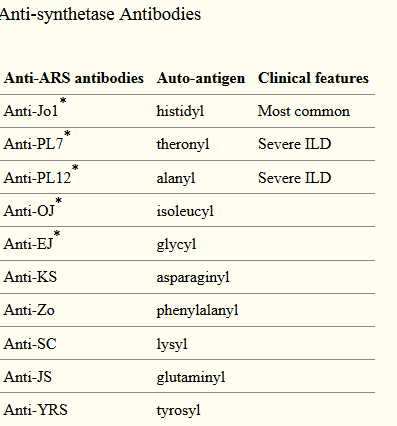

 Source: NEJM, Grepmed
Source: NEJM, Grepmed